Discussion
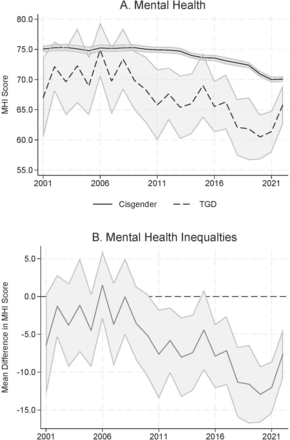
Our findings show that over the 22-year period from 2001 to 2022, TGD respondents had worse mental health than cisgender respondents, with a trend of widening inequalities from 2010 onwards. From 2010, adjusted MHI Scores were 5–13 points lower for TGD individuals relative to cisgender counterparts, even when controlling for potential confounders. Given that a change in MHI Scores of 4–5 points is clinically meaningful,16 this finding represents a substantial and clinically relevant difference in mental health between TGD and cisgender Australians.
Our findings reinforce a growing body of research which has reported poorer mental health outcomes among gender-diverse communities.4 The findings also align with a recent longitudinal study in the USA which found that TGD inequalities in the number of poor mental health days were widening between 2014 and 2021.9 Given gender-based stigmatisation and discrimination have deleterious effects on mental health,21 these results are also consistent with a survey which found that exposure to antitrans rhetoric and interpersonal discrimination among TGD Australians had increased in recent years.22
The results of this study should be interpreted within the context of several important limitations. First, our sample only identifies individuals reporting gender identity in 2022, since that was the first time this question was asked in the HILDA Survey. As such, we were unable to examine the prospective impact of changes in gender identity on individuals’ mental health. This retrospective assignment further hinders our ability to account for the fact that gender identity and expression may be non-linear for some TGD individuals.23 This should be investigated as and when new waves of HILDA become available. Further, this approach necessitates that our sample is restricted to individuals who participated in wave 22 of the HILDA Survey. Consequently, we have larger samples in more recent waves, with only about half of the sample participating in the initial waves. Given potential attrition in the survey over time, it is possible that there could have been changes in the estimated results should gender minorities have been more likely to drop out of HILDA. Stigma surrounding TGD identity could also hinder reporting and thus identification of TGD respondents in our sample. The framing of the gender identity question in HILDA also excludes other identities including individuals who are questioning or not ‘out’ as TGD. Given the lack of collection of gender identity within population-level surveys,10 it is difficult to compare the TGD sample in HILDA to other ‘representative’ samples of TGD in Australia. Should national data collections on gender diversity improve, there will be scope to revisit such analyses in the future. Further, the limited sample size of TGD respondents in HILDA makes it difficult to conduct robust subgroup analyses to further understand which individuals are at heightened risk of poorer mental health. For these reasons, we used adjusted models that included a range of demographic and socioeconomic characteristics, rather than examining trends in mental health inequalities through disaggregation of specific population characteristics. Finally, it is important to acknowledge that, with this sample size, it is difficult to fully separate out the difference in mental health between cisgender and TGD individuals from other characteristics, such as age. This is a particular challenge as young people have poorer mental health24 and, as we demonstrate, are much more likely to be TGD. Nevertheless, when we restrict our sample to younger populations, we observe the same trends in widening TGD mental health inequalities. Collection of TGD identities and mental health in comprehensive whole-of-population data, such as the Census, will be essential to investigate this with greater precision.
Despite these limitations, the present study boasts several strengths and is the first to provide empirical evidence on temporal trends in TGD-cisgender mental health inequalities in Australia. In particular, the external validity of this research is bolstered by the large and nationally representative sample over a long period of time, from 2001 to 2022. To our knowledge, this represents the longest temporal trends analysis for TGD populations globally and is the first to document temporal inequalities using a clinically validated measure of mental health. Further, the comprehensive and longitudinal measures on social and economic factors captured within the HILDA Survey enable us to control for a dynamic set of important confounding characteristics that could impact mental health.
Altogether, these results provide important and context-specific policy insights for Australia. According to the LGBT Equality Index, Australia is the nineteenth most LGBT-friendly country in the world—seven places ahead of the USA.8 In recent years, there have been vast improvements in rights and protections for gender minorities in Australia, including bolstering antidiscrimination protections (eg, the 2013 Sex Discrimination Amendment), removal of ‘forced divorce’ provisions after transitions prior to Marriage Equality in 2017, and improvements in accommodating gender diversity in official identification (eg, ‘X’ category in passports without requiring sex reassignment surgery or amended birth certificates since 2011).8 However, despite this progress, our results suggest that these have been insufficient to ameliorate gender minority mental health inequalities, particularly in recent years.
There remain substantial human rights challenges for TGD Australians. It is highly likely that structural factors are contributing to these mental health inequalities. For example, although a substantial body of research has shown that access to gender-affirming care is associated with better mental health outcomes, including improved quality of life and reduced symptoms of depression and suicidal ideation among TGD populations,25 26 there is inadequate and inequitable access in Australia.5 Many facets of gender-affirming care (eg, surgeries, speech therapy) are still not publicly funded through Australia’s universal health insurance scheme5 and thus patients must self-fund and face substantial out-of-pocket costs to access this care. More broadly, TGD-cisgender mental health inequalities could be exacerbated by limited supply of specialty mental healthcare providers in the Australian context.5 Scarce supply could make it more difficult for TGD Australians to find inclusive and affirming psychological care.27 Indeed, unmet healthcare needs have been cited as a key issue among gender minorities.4 Improved access to affirming care is therefore likely to play an important role in reducing TGD-cisgender mental health inequalities.
Ultimately, more empirical research on the pathways driving gender minority mental health inequalities is needed to help design and deliver effective and targeted policy solutions. Robust and well-powered sample sizes in population-level data sets will be essential to carry out such research. In particular, the Standard for Sex, Gender, Variations of Sex Characteristics and Sexual Orientation Variables, 2020 (‘2020 Standard’)28 29 should be included in population-based surveys, including in subsequent waves of the HILDA Survey and in Australia’s Census of Population and Housing (conducted every 5 years). This would enhance our understanding of how prospective changes in gender identity influence mental health and enable broader analyses that could be stratified by additional gender subgroups, such as non-binary identities. Should the 2020 Standard be included in the 2026 Census, there will also be scope to empirically investigate the drivers of mental health inequalities, including healthcare utilisation, through data sets such as the Person Level Integrated Data Asset.30 Inclusion in large population-level surveys would also facilitate subgroup analyses (eg, by age, remoteness, socioeconomic position) to understand which population groups should be explicitly targeted in policy response. Nevertheless, these results suggest the need for immediate policy action for this important public health issue to reduce clinically important and widening inequalities in TGD mental health.